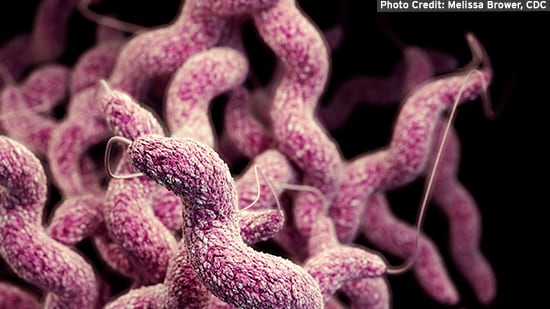
Campylobacter
WHAT IS CAMPYLOBACTER?
Campylobacteriosis is caused by Campylobacter jejuni, one of the most common bacterial causes of acute bacterial diarrheal illness worldwide. Cases of campylobacteriosis are generally isolated, random events, but outbreaks affecting several people can also occur.
The Centres for Disease Control estimates that Campylobacter affects over 1 million people every year in the United States, approximately 100 of whom die from the illness. An estimated one in 1,000 cases of campylobacteriosis leads to Guillain-Barré Syndrome, a neurological ailment resulting in paralysis of extremities.
WHAT ARE THE SYMPTOMS?
Campylobacteriosis typically lasts about one week with the common symptoms of diarrhea, cramping, abdominal pain and fever appearing two to five days after exposure to the organism. In some cases, there may be bloody diarrhea with nausea and vomiting. In immunocompromised people, the organism may spread to the bloodstream and cause a serious infection. Typically, illness occurs more frequently in the summer months than in the winter.
HOW IS IT TRANSMITTED?
Transmission of the organism to people usually occurs from consumption of raw or undercooked poultry (primarily), meat and unpasteurized milk. Cross-contamination of raw to cooked items can also be a contributing factor to illness. The bacterium is not typically spread from person to person, although this can happen if the infected person is producing a large quantity of diarrhea. Fewer than 500 Campylobacterorganisms can cause illness in humans.
Some people can acquire infection from contact with pets, as many animals asymptomatically carry the pathogen in their intestinal tract and excrete Campylobacter in their feces. This more commonly occurs when one has contact with the contaminated stool of a symptomatic dog or cat.
HOW IS IT CONTROLLED?
Proper cooking and prevention of cross-contamination are essential for control of Campylobacter. Incorrect hygienic practices in the kitchen, such as using utensils and cutting boards to prepare raw poultry followed by the preparation of ready-to-eat foods, can cause cross-contamination and illness. Poultry processors are increasingly implementing stringent sanitary practices to reduce Campylobacter incidence in flocks and in manufacturing facilities.
FDA and USDA cleared poultry antimicrobial carcass treatments have been shown to reduce but not eliminate Campylobacter on poultry.1 Use of such treatments must meet specific regulatory requirements. The organism is very sensitive to dry conditions and is unable to survive in foods with a water activity below 0.97.
Campylobacter can grow from 32 - 45°C, pH 4.9 – about 9, and water activity >0.987.2The organism requires a reduced oxygen atmosphere for growth, and its numbers are reduced on raw meat with freezing.
For assistance with this topic or other food safety questions for your operation, please Contact Us.
REFERENCES AND FURTHER INFORMATION
1Arritt, et al. 2002. Efficacy of antimicrobials against Campylobacter jejuni on chicken breast skin. Journal of Applied Poultry Research. 11(4):358-366
2International Commission on Microbiological Specifications for Foods. Microorganisms in Foods 5, Microbiological Specifications of Food Pathogens. Blackie Academic and Professional, New York. 1996.


